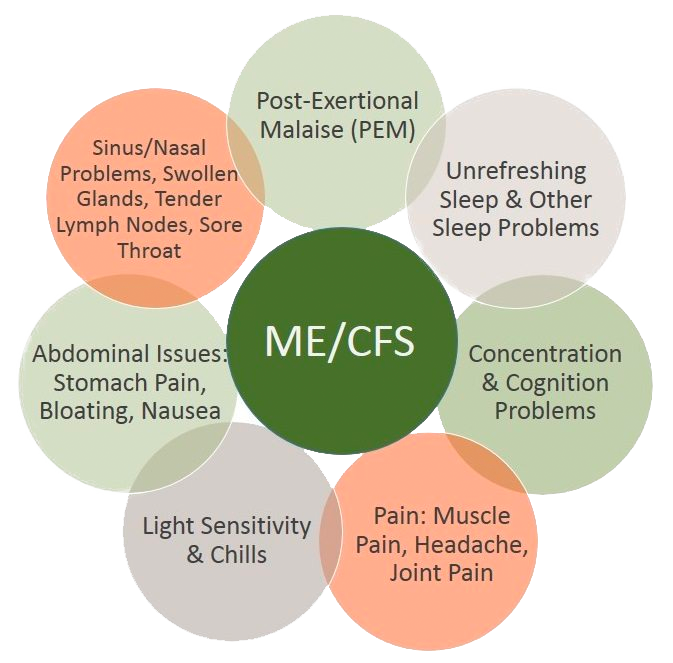
When I was 21 and finishing up my first semester of law school, I got a flu with a fever. So did my mother and sister. I don’t remember who got it first, but it started just after Thanksgiving and we were all still feeling rough by New Year’s. Then it was the end of February, and we still felt fatigued, didn’t sleep well, had gastrointestinal pain and headaches. We went to our family doctor; it was not mono, or anything else he could think to test for. Over time, we also developed a rash on the face, sinus headaches, and “picture skin,” where if any of us scratched ourselves, the skin would create a red, raised line that lasted for an hour or more.
Eventually, the doctor diagnosed Chronic Fatigue Syndrome, which is now more commonly known as ME/CFS. Even now, it is difficult to detangle ME/CFS from lupus or fibromyalgia or other autoimmune conditions, all of which are poorly understood and diagnosed by tests and symptoms that may or may not exist for every sufferer and are never definitive. I’m still not entirely sure that we all had CFS or that I, as the only one of us still living, have it now. What I do know is that in early 2020, just a couple of months after my sister died of cancer, I finally had to acknowledge that my hands and feet ached all the time. I started to see various doctors, including rheumatologists, neurologists, and cardiologists. Additional symptoms popped up: my toes moved involuntarily, my fatigue (which had waxed and waned for 30 years) got worse, my feet and fingers swelled, especially in the heat. It was a funhouse of symptoms, and none of the doctors felt they could diagnose anything in particular.
Three years later, after trying everything from a gluten-free diet to low-dose naltrexone to hormone replacement therapy, I heard about Ozempic. Could losing weight help me, even a little bit? Maybe my joints would hurt less, my muscles not feel as weak? Maybe this drug, which works by either mimicking or triggering (I haven’t been able to understand which) the hormones that tell our brains that we’re full, would help me cut down on sugar, the one foodstuff everyone agrees is inflammatory?
Before I got CFS, I was an athlete. Not an elite athlete, but I played softball, volleyball, and racquetball for fun. I rode my bike for miles in the country outside the town where I grew up and went to college. I took long campus walks with friends and boys, talking late into the night.
After I got sick, my body became my enemy. It was me versus my body, every day. Fatigue makes it difficult to think clearly, and pain makes you tired. I was in a field that involved a lot of thinking—poet, writer, and teacher—so I fought my body to do what I wanted to do. Grading papers was not merely the exercise in willpower that it is for every teacher, the slog of writing the same comments over and over; for me, it was also about ignoring the pain in my head or my stomach, pinching myself and binging sugar-loaded snacks to stay awake (like I often did on long solitary drives), and reminding myself that the students were not responsible for my body’s insolence.
Don’t get me wrong—I love teaching with all my heart, and I feel lucky that my chosen field did not require physical health. But I fought to do what I loved. I, like everyone I know with chronic illness, became a warrior.
So far, what Ozempic has done is to take the edge off my cravings. It’s like when you have a bad headache and take a couple of aspirin; it doesn’t make the headache go away, but you’re not thinking about that pain every second anymore. I’m still on the low starting dose, so I’m hoping the food cravings (oh chocolate, my chocolate) continue to diminish. I’m just ready for something about this interminable war between mind and body to be a little bit easier.
p.s. I’ve just learned about Notes here on Substack, and they look fun and interesting. I’ve posted a link to a fascinating podcast episode in which a neuroscientist talks about the brain and processed food; it’s really worth listening to.